Musculoskeletal pain affects the locomotor system – muscles, joints, bones, tendons, and ligaments. Mobility, dexterity, and functionality are affected when the musculoskeletal system is limited. While musculoskeletal pain rarely causes death, it is the leading cause of disability in four out of six WHO regions last 2017. (1) Globally, twenty to thirty-three percent of the population lives with musculoskeletal conditions.
The prevalence of musculoskeletal pain increases as we age. Chronic musculoskeletal pain results in fatigue and poor productivity. (2) it is also detrimental to the quality of life because it hinders daily activities. Musculoskeletal disorders have burdened one-third of all workers’ compensation costs. (3) In a year, 45 to 54 billion US dollars are spent on musculoskeletal disease. (3) Treatment of chronic diseases is very damaging in the lives of those with musculoskeletal pain and that is why a good investment is to look for the best ways to treat it.
Table of Contents
What is Prolotherapy?
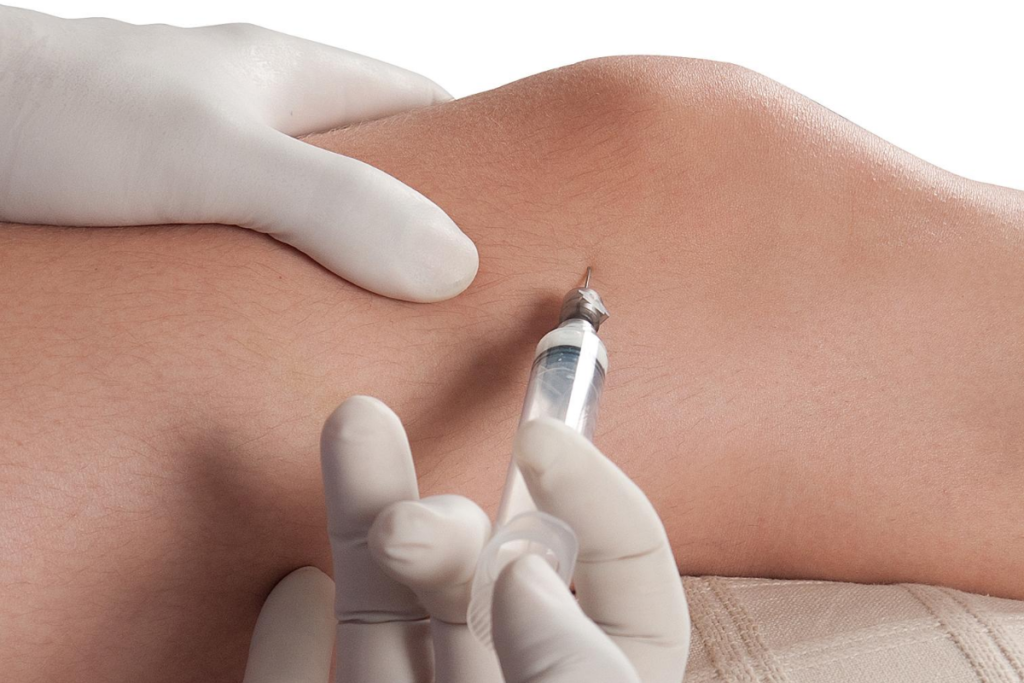
Hippocrates was the first to describe the intentional provocation of scar formation by injuring the shoulder joint in unstable shoulders. (4) Prolotherapy dates back to almost a century ago. In the 1950s, it was formalized by George Hackett, a general surgeon, wherein he claimed that prolotherapy had an 82% cure rate. (4) George Hackett said that out of his 1600 patients with back pain, he cured 1312 with the use of prolotherapy alone (4).
Tendons and ligaments are structures that have a poor blood supply. This delays healing when there is tissue injury. Our nutrition, lifestyle habits, sleep, age, and other medical conditions affect our body’s ability to heal.
In prolotherapy, the regeneration and repair of the cells in the tissue injury is the focus. Prolotherapy is a nonsurgical, complementary, and alternative medical therapy that introduces a small volume of irritant or a sclerosing agent to a ligament or joint for the treatment of chronic musculoskeletal pain. (5) (6) (7) It is also known as non-surgical ligament and tendon reconstruction and regenerative joint injection. (8)Prolotherapy is often used in the knees, hips, shoulders, elbows, ligaments, and joints. A variety of techniques are performed depending on the problem presented. No specific prolotherapy guidelines have been established.
Where is Prolotherapy Useful?
Prolotherapy is generally used for those with chronic musculoskeletal pains. Arthritis, myofascial syndromes, and chronic sprains and strains are also indications of prolotherapy. Other conditions wherein prolotherapy is used are the following:

Medial and lateral epicondylitis of the elbow, knee, ankle, and shoulder
Epicondylitis is a condition where the tendons of the bones are overloaded by continuous repetitive movement. Epicondylitis of the elbow is also called tennis elbow. Repetitive strenuous activity to the areas such as the elbow, knee, ankle, and shoulder can cause inflammation and pain. These can be managed by prolotherapy.
Tendinosis and tendinopathies
Tendinosis is the degeneration of a tendon because of chronic or long-term overuse. When tendons are used repeatedly, it will cause injury and pain. Tendinopathies and tendonitis are often seen in older people. Examples of tendons often affected are those in the shoulder, elbow, wrist, hip, knee, and ankle.
Musculoskeletal pain related to osteoarthritis
Osteoarthritis is a degenerative disease that is made by the wear and tear of the body. This may be in different locations such as knees and joints of the fingers. Pain from osteoarthritis can be relieved by prolotherapy and other regenerative pain management therapies like trigger point therapy, platelet-rich plasma therapy, perineural therapy and a lot more.
Other joint pains
Conditions that involve ligaments and joints are the target of prolotherapy since it can help improve pain significantly and can let you live a normal, pain-free life.
Why Does Prolotherapy Work?

Theories on how prolotherapy works remain unclear but collectively, the proposed mechanism suggests that injection of a sclerosing agent, most commonly dextrose, causes local cell deaths from its direct trauma to the site. (6)This is then acted upon by the inflammatory cascade.
Inflammation is an initial reaction but once it subsides, growth factors will remain for weeks to stimulate wound healing and collagen deposition. Once the site is healed, it becomes more stable and pain-free, thus a more long-term effect is achieved.
Other proposed ways by which prolotherapy could bring about healing and stabilization is as follows:
- Mechanical damage made by the needle injury to the body stimulates the inflammatory cascade which is also in charge of releasing growth factors. A growth factor is a substance in the body that has a role in the regulation of wound healing. (9) Because growth factors are released in the area, the damaged site has an increased healing ability.
- The agent introduced to the site through injection is considered as an external fluid and this fluid, due to its volume, causes cell compression. The hypertonic (highly concentrated) dextrose is also believed to cause cell dehydration and osmotic rupture at the site leading to tissue injury. (7) This injurious event also stimulates growth factors to initiate wound healing giving the same effect as the needle injury theory.
- Chemicals from the agent injected trigger production of collagen through inflammation still mediated by cytokines (signaling molecules communicating inflammation) and growth factors. (9)
- The impulses received by nociceptors (receptor of pain) are stabilized by the use of the agent which also leads to reduced pain. (9)
- Local blood flow is often disturbed in those suffering from arthritis. In prolotherapy, the local blood flow is controlled through change in intraosseous (inside a bone/joint) pressure leading to a reduction of pain. A combination of lidocaine and dextrose has longer pain control than lidocaine alone. (9)
- Inflammation produced by the injection of sclerosing agents creates a better environment for hypermobile joints to repair and regenerate. (9)
- The initial lesion in the original tissue damage is disrupted by large volumes of solutions injected. This would again injure the previously healed tissue causing a new wave of inflammatory response and healing process. (9)
All these mechanisms are possible ways of how prolotherapy treats pain and laxity of ligaments. It is also hypothesized that this small ‘therapeutic trauma’ initiates wound healing leading to reduced pain and stabilization of the injury. (10) This treatment procedure makes use of the body’s resources to naturally heal weakened tissues again.
How is Prolotherapy Done?
Prolotherapy is a procedure done by our licensed doctors in hundreds of patients. To give you a better idea on how it is done we have list down the following steps in prolotherapy (11):
- Initially, when you come in due to pain or instability, a thorough history is performed. Our doctors may ask for the signs and symptoms that you have felt and for other medical problems experienced aside from musculoskeletal pain. This is done by our doctor to determine whether prolotherapy is the proper treatment needed. This will also help our doctor weigh in the benefits and risks of prolotherapy as your treatment.
- Initial physical examination is vital before any procedure is done. To localize properly, palpation (a method of feeling with the use of the fingers) is performed by our doctor noting areas of tenderness and the rating of pain as felt by you or your patient. Painful areas are mapped out with dots using a marker. Explanation of the procedure is then discussed so that you could better understand what will happen. Specific details such as the sclerosing agent used are discussed. Others may use dextrose alone as it enhances collagen synthesis. A combination of dextrose and lidocaine/procaine (anesthetic for pain control) can also be used. (12) Others make use of sarapine, saline, or, in the recent advances, platelet-rich plasma.
- Once you have understood and you have given your consent for the procedure, proper preparation of the site is made. Instruments to be used are prepared. Our doctor will wear his gloves and start by cleansing the site without removing the markers. This technique prevents contamination of pathogens during the procedure and avoiding infection.
- The solution of choice is then injected in the sites deemed as important by our doctor. These injection sessions are spaced out to every 2 to 4 weeks depending on the severity of your condition. (13)
- After the injection sessions, we do our Prolotherapy shots once a week for a total of 3 weeks. (13)
Initially, symptoms of pain and soreness may be aggravated by the injection. (15) This is normal as inflammation is produced to stimulate tissue repair. Massage and hot compress may be done to help relieve the pain. If the pain still persists, painkillers without anti-inflammatory effects may be taken.
Few weeks after the treatment, the initial stabilization effect of prolotherapy will be noted. Patients often perceive that sessions following the first treatment do not give the expected relief. This is mainly due to the increase in activities done by the patients. Once you resume your previous activities, your body may not be at its top shape. Healing is a process and it differs greatly per person. Others may feel immediate relief while some may feel the relief later on.
Contraindications for Prolotherapy
There are few contraindications for prolotherapy. Absolute contraindications mean that it should never be done as it may lead to a life-threatening situation.
On the other hand, relative contraindications mean that proper precautions should be made when prolotherapy is performed with the existing conditions.
Absolute contraindications of prolotherapy are:
- Acute infections such as cellulitis, local abscesses, and septic arthritis (6)
- Immunocompromised patients – those with cancer and are undergoing chemotherapy, those undergoing hemodialysis, transplant patients and those taking immunosuppressants (drugs subduing the immune system).
- Malnourished patients.
- Patients with allergies to the local anesthetic or any of the solutions used.
- Patients on anticoagulants who have high INR (international normalized ratio).
- Complete ligament or tendon tear.
Relative Contraindications of prolotherapy use:
- Acute gouty arthritis
- Acute fracture
Side Effects of Prolotherapy
Side effects of prolotherapy are classified either due to the substance used or may be needle-related. Other side effects are dependent on the skill of the physician and the severity of the disease.
Needle related side effects could occur due to damage produced in the site of injection. Peripheral nerve injury can lead to loss of sensation or motor function.
The infection of the joint may also be present if the proper aseptic technique was not performed. This is why it is important to see a licensed doctor who has experience and training in doing prolotherapy.
Spinal headache is also experienced when the site of injection is near the spinal canal. In injections near the thorax, pneumothorax may occur. Bruising may also be seen due to the injections. (15) Possible outcomes after prolotherapy is immediate pain after injection, bleeding from the site of injection, and post-therapeutic muscle spasm. These are all normal and will go away after a few hours.
Substance-related side effects are mainly due to the solution used in prolotherapy. After injection, stiffness may be experienced up to 3 days. (4) People with hypersensitivity to dextrose may develop rash, hives, chest tightness, and wheezing, if this occurs, contact your doctor ASAP. Lightheadedness and nerve damage are also possible when there is hypersensitivity.
Complications of Prolotherapy
A small number of prolotherapy-related complications have been recorded. These complications are often related to side effects of perispinal injections on the neck and back. Prolotherapy procedures are relatively safe if performed by skilled physicians. Manipulations of the spinal cord area and neck should always be done with proper precaution.
Summary
Prolotherapy has long been practiced and it has brought relief to patients suffering from musculoskeletal pain for years. With its safety and effectiveness, it is a natural pain management procedure that may bring you the ease you have been looking for whether for acute or chronic pain.
As a recap, we have discussed the following in this blog article:
- What is Prolotherapy?
- Where is Prolotherapy Useful?
- Why Does Prolotherapy Work?
- How is Prolotherapy Done?
- Contraindications for Prolotherapy
- Side effects of Prolotherapy
- Complications of Prolotherapy
If you want to learn more about prolotherapy or are wondering if it is for you, you can contact us or book an appointment with us here.
References:
- World Health Organization (2019). Musculoskeletal conditions. Retrieved from https://www.who.int/news-room/fact-sheets/detail/musculoskeletal-conditions#:~:text=While%20the%20prevalence%20of%20musculoskeletal%20conditions%20varies%20by%20age%20and,with%20a%20painful%20musculoskeletal%20condition.
- Daneshmandi, H., Choobineh, A. R., Ghaem, H., Alhamd, M., &Fakherpour, A. (2017). The effect of musculoskeletal problems on fatigue and productivity of office personnel: a cross-sectional study. Journal of preventive medicine and hygiene, 58(3), E252–E258.
- Roux, C.H., et al. (2004). Impact of musculoskeletal disorders on quality of life: an inception cohort study. Annals of the Rheumatic Disease. 2005(64), 606-611.
- Cusi, M. (2012) Prolotherapy. Retrieved from http://www.orthosports.com.au/pdf-download/Prolotherapy.pdf
- Distel, L. M., & Best, T. M. (2011). Prolotherapy: a clinical review of its role in treating chronic musculoskeletal pain. PM &R : the journal of injury, function, and rehabilitation, 3(6 Suppl 1), S78–S81. https://doi.org/10.1016/j.pmrj.2011.04.003
- Rabago, D., Slattengren, A., &Zgierska, A. (2010). Prolotherapy in primary care practice. Primary care, 37(1), 65–80. https://doi.org/10.1016/j.pop.2009.09.013
- Siadat, A. H., &Isseroff, R. R. (2019). Prolotherapy: Potential for the Treatment of Chronic Wounds?. Advances in wound care, 8(4), 160–167. https://doi.org/10.1089/wound.2018.0866
- The American Osteopathic Association of Prolotherapy Regenerative Medicine (n.d.). What is prolotherapy? Retrieved from https://prolotherapycollege.org/what-is-prolotherapy/
- Park, J. W., Hwang, S. R., & Yoon, I. S. (2017). Advanced Growth Factor Delivery Systems in Wound Management and Skin Regeneration. Molecules (Basel, Switzerland), 22(8), 1259. https://doi.org/10.3390/molecules22081259
- Sanderson, L. M., & Bryant, A. (2015). Effectiveness and safety of prolotherapy injections for management of lower limb tendinopathy and fasciopathy: a systematic review. Journal of foot and ankle research, 8, 57. https://doi.org/10.1186/s13047-015-0114-5
- Baehnisch, G. (2010). Prolotherapy tips for beginners: how i started with prolotherapy. Journal of Prolotherapy. 2(2)
- Fletcher, J. (2017). What is prolotherapy and what is it used to treat? Retrieved from https://www.medicalnewstoday.com/articles/320330
- Baehnisch, G. (2010). Prolotherapy tips for beginners: how i started with prolotherapy. Journal of Prolotherapy. 2(2)
- Mooney, V. (2001). What are the current indications for prolotherapy? Retrieved from https://www.spine-health.com/treatment/injections/what-are-current-indications-prolotherapy
- Dagenais, S., Ogunseitan, O., Haldeman, S., Wooley, J. R., & Newcomb, R. L. (2006). Side effects and adverse events related to intraligamentous injection of sclerosing solutions (prolotherapy) for back and neck pain: A survey of practitioners. Archives of physical medicine and rehabilitation, 87(7), 909–913. https://doi.org/10.1016/j.apmr.2006.03.017

