In 2016, an estimated 20.6% or 50 million Americans experienced chronic pain. (1) Pain is not only physically and mentally distressing but it limits the life and work activities of each individual and no one deserves to live a life in pain.
Table of Contents
What is Trigger Point Therapy?
Trigger point therapy has been around since the 1940s when Dr. Janet Travell first coined the words “trigger point”. (2) Dr. Travell is well known because she treated President Kennedy’s back pain. She became the first female personal physician to the president in 1960. Since that time, trigger point became well known and multiple specialists have adopted and studied the theory of trigger point and how to manage it.
So what is the deal with trigger point and trigger point therapy and why should you know more about it?
It has been estimated that about 23 million people in the United States (3) have one or more disorders of the muscles and the skeletal system and this disability is causing a heavy burden physically, emotionally and financially to these people.
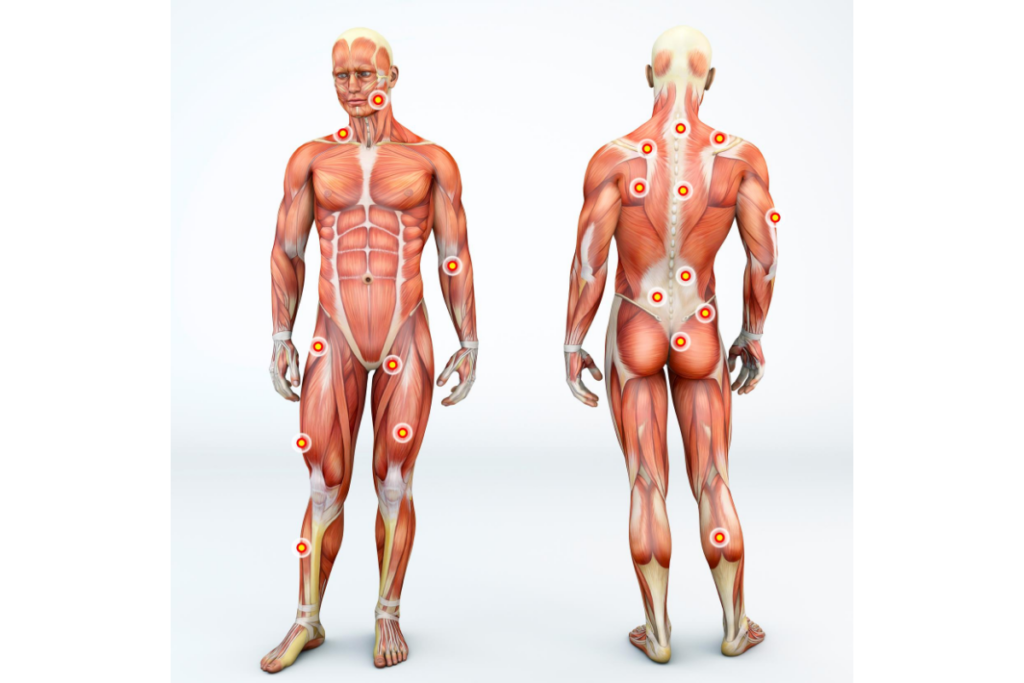
Trigger points are hyperirritable spots located in areas of the skeletal muscles. The skeletal muscles are the muscles that you can move voluntarily like the ones found in your hamstrings, biceps and all over your arms and legs.
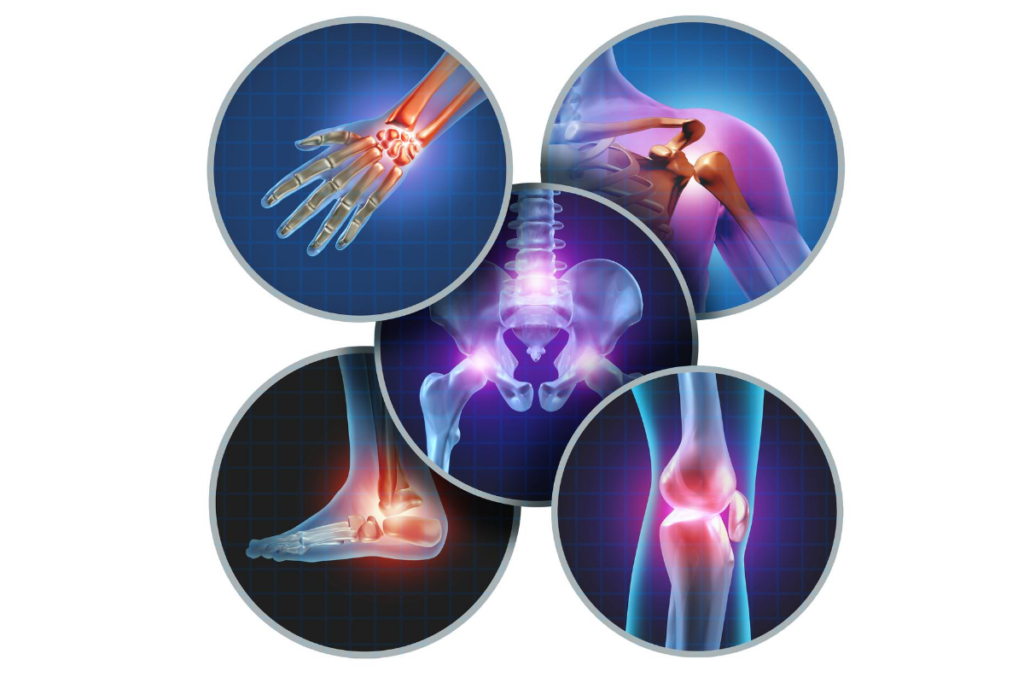
These trigger points can produce pain locally that can cause significant decreased in range of motion— affecting even the simplest movements in your everyday life. Trigger point pain may manifest as pain in the neck, shoulder, leg or foot but it can also manifest as pain in the temples or head (tension headaches, migraine) or even in the jaw.
Palpating the area where the bundle of muscle fiber is found can cause direct pain in a certain zone which we refer to as referred pain. You will notice that when palpating these areas, they may be harder than usual and may become tense when pressure is placed.
Why do I have pain in my trigger point?
There are many reasons why you may have trigger point pain and multiple types of research have the same explanation: trauma, be it micro-trauma or repetitive trauma to the area, poor posture, lack of exercise, poor sleep or joint patterns, and even poor nutrition, are all causes of trigger point pain. (4)
They have also described that repetitive stress on specific areas of the muscle may cause trigger points. Examples are having poor posture on the back, repetitive use of the finger muscle when typing or using a mouse, and even repetitive pressure on the sole when walking can all be predisposing factors in getting trigger points. Sports injuries like a tennis elbow or a golf shoulder are also common causes of trigger point pain.
These trigger points can either be active or latent.
Active trigger points are those causing you pain even while at rest. You may be lying down in bed doing nothing but your lower back keeps throbbing, or your elbow keeps on waking you up at night— these are all active trigger points, they let you feel pain even when you do not move or touch the areas involved.
When palpated these are also very painful or tender, there will also be referred pain when these areas are touched and the pain can spread all throughout the different parts near the trigger point.
Latent trigger points are those painful only when palpated or touched. For instance, your trigger point in the biceps may only hurt when squeezed or pressed on but when doing nothing; it does not disturb you at all.
What are the symptoms of trigger point pain?
As mentioned, a trigger point will present as pain on specific muscles or muscle groups that have tenderness on palpation or at rest. Referred pain is important in trigger point since it will differentiate it from a tender point.
A tender point only has local tenderness occurring in multiple muscles that may be asymmetric in location. It does not cause referred pain but can cause an overall increase in pain sensitivity in the body.
A trigger point also has local tenderness but it usually involves a taut band (or a tensed band of muscle that is irritable and is connected to the attachment of the involved fiber). A jump sign is frequently present with a local twitch response.
A jump sign is when a person becomes startled by the pain caused by applying pressure on the affected trigger point whereas a local twitch response is a dimpling of the overlying muscle when pressure is applied.
Trigger points often happen in a single or multiple muscle areas, and occurs in a skeletal muscle and has referred pain. (5) Referred pain is an important distinguishing feature because as mentioned earlier, this is not present in a tender point.
Trigger point pain is often persistent and results in a decreased range of motion (like in a tennis elbow where there is difficulty extending and flexing the arm). Common areas affected are the muscles of the shoulders, neck, back and even the pelvic area. Trigger points usually do not have symptoms like joint swelling or neurologic deficits (like decreased sensation or numbness). (6)
How will I get evaluated?
Evaluation of trigger points will be done by our doctor. They will perform a complete physical examination where the problem areas will be inspected and palpated. Areas with trigger points are usually firm or harder than the usual muscles when palpated and there will be tenderness on the area. You may also be asked to follow a series of tests for a range of motion like extending or flexing your arm or moving them from side to side.
Currently, no laboratory tests have been established in diagnosing trigger point but ultrasonography, electromyography, thermography, and muscle biopsy are being studied to assist in its diagnosis.
Is there a treatment for my pain?
Since trigger points are usually caused by overuse or stress injury to the muscles, these activities are often avoided or eliminated completely. Medications for trigger points may include analgesics like ibuprofen or muscle relaxants.
Acupressure, acupuncture, application of ice or heat, electrical nerve stimulation may also be done to help decrease pain. Other regenerative treatments like platelet-rich plasma therapy that can help with pain are also available.
Manual methods may also be done to help train the patient to manage the pain and work towards better functioning but this method usually requires multiple visits and may not be as effective at trigger point injections.
Trigger point injection and dry needling is an effective approach that could provide instant relief to patients suffering from pain. It is indicated for patients that have trigger points that generate a twitch response to pressure or those with moderate to severe pain.
Trigger point injection may be done with procaine or lidocaine or even through dry needling. (7) One study showed that dry needling may be as effective as injecting an anesthetic medication on the trigger point to help alleviate pain. (8)
What happens during the procedure?
Before starting the procedure, you will need to be evaluated for bleeding tendencies.
You may be asked for the history of medications that you are taking that may cause bleeding like warfarin, aspirin, clopidogrel, or anticoagulants like rivaroxaban, apixaban or dabigatran. If you are taking any of these medications, it would be best if you would contact us first prior to your procedure.
You will be placed in a comfortable position, depending on where the area of pain is located. Needles used will depend on the site we need to reach but rest assured that these needles will cause minimal pain if any.
Solutions used are commonly lidocaine, procaine or corticosteroids depending on your need. Don’t worry, you will be evaluated and assessed prior to getting the injection.
Once your trigger point has been located, the skin will be cleansed thoroughly with alcohol or betadine. The procedure will be done aseptically, to make sure that everything that touches your skin is clean and free of bacteria.
When the needle is about to pass your trigger point, you may feel a sharp pain or muscle twitch when the needle comes in contact with the taut muscle band. The medication will then be introduced after ensuring that no blood vessel has been hit.
With the trigger point injection, you will feel instant relief from pain or there could be numbness on the site. This is normal since an anesthetic is being given. It may take several trigger point injections to totally be free of pain but this will always depend on its severity, how long it has been present (chronicity) or the area affected.
After the injection, the area will be palpated to make sure that there is no pain. Stretching of the muscle group may be done to improve the effectiveness of the trigger point injection as mentioned in one study. (9)
Are there contraindications to trigger point therapy?
Contraindications of trigger point therapy are any of the following (10):
- Bleeding disorders like haemophilia, thrombocytopenia (any disorder that causes easy bruising or bleeding) or taking anticoagulants like warfarin, heparin, dabigatran, rivaroxaban, enoxaparin, fondaparinux, etc. (contact our clinic first if you are taking any of these medications, it may be put on hold for a few days prior to your procedure).
- Intake of aspirin the past three days prior to injection.
- Allergy to anesthetics like lidocaine or procaine.
- Acute muscle trauma
- Systemic or local infection
Are there any complications to trigger point therapy?
Complications of trigger point therapy are often mild and are expected. Post injection site pain may be felt which can be treated with analgesics. Hematoma or bruising may be present but an ice pack can help reduce it.
Conclusion
Trigger point therapy has become a promising solution to pain especially when there are no indications for surgery like in the case of one study where trigger point injections were given to a patient with lumbar disc hernia (11). It is also beneficial for patients who have been suffering from pain unresolved by medications for quite some time.
As a recap, we have discussed the following in this article:
- Trigger Point Therapy— What is it, really?
- Why do I have pain in my trigger point?
- What are the symptoms of trigger point?
- How will I get evaluated?
- Is there a treatment for my pain?
- Are there contraindications to trigger point therapy?
- Are there any complications to trigger point therapy?
If you have been suffering from pain and want relief and improvement, you may contact us for more information.
References:
- Dahlhamer, J., Lucas, J., Zelaya, C., Nahin, R., Mackey, S., DeBar, L., Kerns, R., Von Korff, M., Porter, L., & Helmick, C. (2018). Prevalence of Chronic Pain and High-Impact Chronic Pain Among Adults – United States, 2016. MMWR. Morbidity and mortality weekly report, 67(36), 1001–1006. https://doi.org/10.15585/mmwr.mm6736a2
- “Trigger Point Therapy .” Gale Encyclopedia of Alternative Medicine. . Retrieved July 14, 2020 from Encyclopedia.com: https://www.encyclopedia.com/medicine/encyclopedias-almanacs-transcripts-and-maps/trigger-point-therapy
- Imamura ST, Fischer AA, Imamura M, Teixeira MJ, Tchia Yeng Lin, Kaziyama HS, et al. Pain management using myofascial approach when other treatment failed. Phys Med Rehabil Clin North Am. 1997;8:179–96.
- Rachlin ES. Trigger points. In: Rachlin ES, ed. Myofascial pain and fibromyalgia: trigger point management. St. Louis: Mosby, 1994:145–57.
- Alvarez, D. J., & Rockwell, P. G. (2002). Trigger points: diagnosis and management. American family physician, 65(4), 653–660.
- Yunus MB. Fibromyalgia syndrome and myofascial pain syndrome: clinical features, laboratory tests, diagnosis, and pathophysiologic mechanisms. In: Rachlin ES, ed. Myofascial pain and fibromyalgia: trigger point management. St. Louis: Mosby, 1994:3–29.
- Simons DG, Travell JG, Simons LS. Travell & Simons’ Myofascial pain and dysfunction: the trigger point manual. 2d ed. Baltimore: Williams & Wilkins, 1999:94–173.
- Hong CZ. Lidocaine injection versus dry needling to myofascial trigger point. The importance of the local twitch response. Am J Phys Med Rehabil. 1994;73:256–63.
- Zohn DA, Mennell JM. Musculoskeletal pain: diagnosis and physical treatment. Boston: Little, Brown, 1976:126–9,190–3.
- Ruoff GE. Technique of trigger point injection. In: Pfenninger JL, Fowler GC, eds. Procedures for primary care physicians. St. Louis: Mosby, 1994:164–7.

